Rotation Recap: Trauma ICU
To be honest, this rotation was the most challenging one I have faced yet both academically and emotionally. I was prepared for the gruesome injuries, the energy of the trauma bay as vascular access is established and the primary assessment (ABCDEs) is conducted. I was prepared for emergency intubations, exploratory laparotomies, and the inevitable codes. I anticipated this environment and was excited to be a part of truly exhausting all measures to save a life. What I was not at all prepared for, is what comes after the life is saved, the long road to recovery, and when there’s nothing more that can be done. I learned quickly that in the TBICU, you not only admit patients but patients’ families, their moms and children and siblings and spouses. Sometimes, family cannot be located for several days or weeks and the hospital’s ethics committee would have to act as a patient’s medical decision maker. I found both situations profoundly sad, although I was also often reminded of the healing power of love. I truly believe I saw a mother will her son to live and thrive, as he went from a dismal prognosis to chatting with staff and beginning physical therapy during my month there. I saw the wife of an older gentleman who never left his room and dutifully listened to us rounding on him each morning, waiting patiently as students of every kind, pharmacists, nurses, residents, and attendings rattled off high-speed analyses of her husband’s condition in a language she didn’t understand. She wrote everything down day by day in a notebook and learned to understand key lab values and assist the nurses tell us how he did overnight.
I always thought of myself as a Christina Yang to the core but this month really brought out the Izzie Stevens in me.
Before this rotation, almost all of my patients had been mostly self-sufficient, capable of speaking for themselves and making their own medical decisions, and there was little to no concern of death. I did not realize how different these circumstances would make my interactions with these patients and their families. I didn’t know how long I would think about the patients after I left the hospital after our 12 hour shifts or while I was falling asleep. What I’m trying to say is that I always thought of myself as a Christina Yang to the core but this month really brought out the Izzie Stevens in me. There is a culture in medicine where we use dark humor to cope with horrific situations, put on a poker face and never let your preceptor see you cry, and say we’re totally okay even if we’re not. If you’re guilty of this like I am, I want you to know that we aren’t meant to feel comfortable with human suffering or tragedy. It’s not supposed to be easy to watch someone cry. Feeling compassion does not indicate that “you’re not cut out for this,” which is how I felt many times. It’s normal, especially if it’s your first time working in critical care.
Okay, if you’ve made it through me being #inmyfeelings and you just came here for the tips, I totally understand. Here goes.
What To Expect
One Liners and Presentations – This part of every morning was pretty classic, traditional medical education. When I got there, I was responsible for one (and later 2 and 3) patients to pre-round on. This meant reviewing what happened overnight w/ the nurse, reviewing labs, ventilator settings, antibiotics, neuro status, etc. and getting all the facts straight for both a “one-liner” (more on that later) and a formal head to toe presentation. At 8 AM, all the attendings, residents, and students quickly reviewed each patient on the unit and what was happening w/ them. This is where we presented a “one-liner,” which is literally ONE LINE summing up the patient. I will give examples of this later on. If you start rambling, someone WILL cut you off and it WILL be embarrassing. After that, the attending, residents, APPs, students, a pharmacist, and the charge nurse began rounds. This is where you present the patient formally to the attending. It’s up to you to figure out how the attending that week likes the presentation. Some like it quick and sweet. Others like meticulous detail. Go figure. Subscribe to my newsletter and receive a copy of the rounding sheet I used, example completed sheet, and tips and tricks for patient presentations! You could always use a notebook but an organized, detailed rounding sheet will make you look and sound like a pro to your attending and you won’t miss a thing!
Being Lost as Last Year’s Easter Egg – (I got that saying from my mom.. Always makes me laugh). But really, for the first entire week I felt like I was on another planet. I didn’t understand the abbreviations, acronyms, or numbers being thrown around as people rapidly ran the list of patients. I felt like I was barely hanging on and kept a running list in my pocket notebook (get one, btw) of things to look up. The list had probably 20 terms on the very first day. If you’re unfamiliar with a term, take it upon yourself to look it up. If you need further clarification, then ask your preceptor. I added a snapshot of my first list (which I added to daily, might I add) to the photos below!
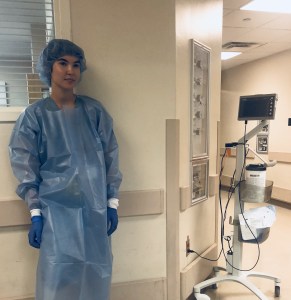
Get In There! (yeah, yeah..) – I carried around a pager that would let me know when traumas were arriving either by ground or air. Sometimes I’d go up to the helicopter and help get patients off or run down to the bay, eagerly put on all my PPE aaaaand stand by while everyone rushed around me, doing their jobs (see pic below). It took a push from my classmate Katie (who basically held my hand through introducing myself to the folks in the bay) before I jumped in and started to help cut clothes off, call out secondary assessments, and start IVs (if the trauma wasn’t too serious). I had a much better time after I broke the ice, asked if I could help, and got my foot in the door of the life-saving business! Don’t wait like I did to jump into the action and then regret not being more hands-on. (PS – Thank you Katie)
How To Prepare
You can’t – Ha, just kidding (kinda). When I touched base with my preceptor before the rotation started, she told me to just bring a good attitude and willingness to work hard and learn. She also said that 80% of ICU care is not really covered in school. It’s very much a learn as you go type thing. If you MUST prepare yourself, this is what I recommend:
If you know an RT, pick their brain – We had a talk on ventilators once somewhere in the ocean of information that was didactic year but I honestly had no idea what to do with them. If you have no idea what it means to say “he’s on pressures at 12 with a PEEP of 8” then you’re not alone. Luckily, one of the PAs at UAB, Jeff, has a famous ventilator talk where he teaches you vent 101 in less than 30 minutes. It was SO helpful, I plan on sharing it with you guys when I get some time! Review the different ventilator settings (spontaneous, SIMV, etc). Also review extubation parameters and contraindications to endotracheal intubation. Lastly, brush up on reading ABGs. Those are very important in this world!
Trache & PEG – At least every day, we sent a patient down for tracheostomy and PEG (percutaneous endoscopic gastrostomy) tube placement. I got to scrub in on a couple of these procedures and they go very quickly. I recommend reviewing the procedures and the indications for them. Both are very common in the critical care setting so it’s good to be familiar. Aside from that, the only other surgeries I saw were ex-laps but if you luck up you can get it on emergency ortho surgeries and neurosurgeries!
Procedure time! – Remember in sim lab when you got to put in central lines, arterial lines, foley catheters, NG and OG tubes, etc. That was so fun, right!? I know I shared my photos intubating those dummies! Now it’s time to recall all that and do it for real! The procedures were my favorite part of the rotation and I got to put in central lines, arterial lines, and perform bronchoscopies and BALs. (Don’t know what a BAL is? Just another thing on your little list of things to look up!) Doing procedures on a real patient is so nerve wracking but thanks to YouTube, you have access to all the how-to tutorials your heart desires.
Access & Tubing – It’s very overwhelming to walk into a room of a patient you’ve not fully reviewed and see a conglomeration of tubes and wires running in every direction. Familiarize yourself quickly with the different types of access people may have (peripheral IV, central line in the IJ, subclavian, or femoral, PICC line, permacaths, trauamcaths, IO access, you name it). Also, people may have PEG tubes, G tubes, J tubes, OG/NG tubes, Dobhoffs, etc. Do a quick review of these and the indications for them. It’ll make your life a tad bit easier. It’s also likely that your attending will ask about lines and how long they’ve been in. Know it! (Or better yet, have a super organized rounding sheet ready).
There are probably a million more things I wish I would’ve known about before starting the rotation but I think this post has gone on long enough. For those of you still reading, WOW! Thank you! If you have any questions or comments, please feel free to drop em below!
Looking for the scoop on other rotations? Check out Emergency Medicine, Inpatient Medicine, Pediatrics, General Surgery, Psyche, Trauma ICU, Cardiothoracic Surgery, Plastic Surgery, Family Medicine, and OBGYN!
Love and light,
Asia